WODURCH WERDEN HÜFTSCHMERZEN VERURSACHT?
Symptome, Diagnose und Behandlungen
Hüftschmerzen können durch eine Verschlechterung des Gelenks, die "Arthrose", beeinträchtigt werden. Sie trifft im Allgemeinen ältere Menschen und eher selten vor dem 50. Lebensjahr bei jungen Menschen.
Die Ursachen können in mehrere Kategorien unterteilt werden:
-
Traumatische Faktoren: schlecht geheilte Verletzungen oder Krankheiten, z. B. eine Luxation.
-
Gefäßfaktoren: Diese Ursachen führen zu Luxationen und anderen Gefäßschäden, die eine Hüftarthrose auslösen können. Ein Beispiel hierfür ist die Perthes-Krankheit, bei der es sich um eine Deformität des Femurkopfes und eine Arthrose aufgrund einer Gefäßinsuffizienz handelt.
-
Angeborene Faktoren: Durch Entwicklungsstörung des Fetus, beispielsweise bei Hüftdysplasie oder durch eine Wachstumsstörung (Perthes-Krankheit bei Kindern).
-
Ungleichgewicht: Zum Beispiel verursacht durch eine Unebenheit oder ungleichmäßige Länge der unteren Gliedmaßen.
Symptome
-
Schmerzen in der Leiste oder Ausbreitung auf das Bein.
-
Steifheit
-
Einschränkungen und Probleme beim Gehen
-
Verlust der Mobilität
Behandlungen
Übergewicht hilft den Gelenken nicht, sie belasten die lebenswichtigen Stützen und können eine Beschwerde sein. Eine geeignete Diät zum Abnehmen wird empfohlen, um die Mobilität zu verbessern.
"Arthrose der Hüften kann operiert werden" Eine sehr wichtige Ressource für Menschen mit sehr fortgeschrittener Arthros e und erheblichen Einschränkungen der Beweglichkeit sowie Schmerzen ist der chirurgische Eingriff.
Hip prosthesis
Hip arthroplasty is a surgery in which the hip joint affected by osteoarthritis, which is a degenerative disease, is replaced, even after a fracture.
Hip joint replacement surgery can be performed using a variety of techniques and approaches. The decision to use one technique or another will be made by the surgeon based on the patient's characteristics.
The main objective of the implantation of a total hip replacement is to improve the patient's quality of life by eliminating pain. The majority of patients who present an indication for total hip arthroplasty are people suffering from osteoarthritis of the hip, which normally appears in people over 50 years of age, regardless of gender. It consists of wear and tear of the cartilage that covers the bone of the joints. The consequences of osteoarthritis of the hip are pain, deformity and loss of mobility, which leads to a significant deterioration in quality of life.
In the initial stages of the disease, conservative treatment is used to palliate the symptoms, trying to preserve the original joint by means of physiotherapy, analgesic-anti-inflammatory drugs, joint infiltrations or weight loss. When pain, deformity and loss of mobility cause limitations in daily life, the only solution to recover quality of life is the implantation of a total hip prosthesis.
Once the specialist doctor gives an indication for hip joint replacement, the patient will make the decision, at all times under medical advice.
The success rate after hip arthroplasty surgery is very high, as it is a frequent surgery. In Spain, more than 30,000 total hip arthroplasties are performed every year.
What does a hip replacement consist of?
The hip prosthesis is an artificial joint that makes it possible to replace a hip affected by degenerative disease, as well as after fractures secondary to falls or accidents.
A hip prosthesis has two main components:
-
Femoral stem or component: part implanted in the femur. The femoral head is adapted to its upper part, with different depths to give more or less length to the operated limb.
-
Cotilus or acetabular component, which is implanted in the pelvis. It is a cup that is impacted into the bone that has been previously prepared to an exact diameter, in such a way that it is fixed to the bone. It can be anchored by pressure or, in the case of very low bone density, by means of a special cement. In our case, we prioritise the use of NO cement.
The hip prostheses currently offered on the market are the result of many years of evolution, offering excellent products in terms of both strength and durability.
The hip replacement operation in Palma de Mallorca
The hip replacement surgery requires a necessary protocol for an intervention with maximum safety and with the highest possible success rate.
It is important in this first consultation that the patient provides all the information related to his or her case (X-rays, reports, MRI scans, etc.). In this way and after the physical examination, the indication for the hip arthroplasty operation will be given or not.
In this first consultation, the patient will be able to ask all the questions he or she may have about the surgery, in order to resolve all their doubts and thus allow them to make an informed decision about whether or not to undergo hip replacement surgery.
Once the decision has been made to carry out the total prosthesis operation in our Prosthetic Surgery Unit, an appointment will be made for the preoperative study, as well as the corresponding consultation with our anaesthesiology specialist. Likewise, a date will be set for the surgical intervention.
Preoperative
The tests to be performed in thepre-operative period for total hip replacement surgery are an electrocardiogram, a complete blood test and a chest x-ray.
The next step is the visit with the anaesthesiologist, who will assess, together with the complementary tests carried out, the patient's general the general condition of the patient, the pathological history and the risk of anaesthesia.
The type of anaesthesia to be used during the operation will be determined.
Our team will teach you some breathing exercises to avoid postoperative problems with anaesthesia postoperative problems with anaesthesia.
Income
The patient will come to the clinic on the scheduled day.
Admission will take place the night before, if the surgery is performed in the morning, or the same day if the hip replacement operation is performed in the afternoon. Once the corresponding documentation has been handed over, the patient will be accompanied to their individual room with a companion's bed where they will remain until the time of the operation. The patient will be showered with special antiseptic gel and dressed in surgical clothing.
The total hip replacement operation step by step
-
In the pre-anaesthesia room, the patient is prepared by inserting a peripheral line, administering a pre-operative antibiotic and, if necessary, shaving the surgical approach site.
-
In the operating theatre, the anaesthetist will administer sedation and spinal anaesthesia, so that the patient does not feel anything during the surgery. In rare cases, general anaesthesia may be used. The anaesthesiologist will remain in the operating theatre at the patient's side during the entire operation, regulating and monitoring the patient's vital signs.
-
Once the patient has fallen asleep, a urinary catheter will be placed.
-
On the operating table, the patient will be positioned in a lateral position and will be supported during the surgery with supports.
-
An incision is made in the hip area 15 to 20 centimetres long and deep enough to expose the joint.
-
The degenerated and worn femoral head shall be exposed and cut with a surgical saw. The femoral canal as well as the acetabulum in the pelvis shall be prepared in such a way that the components are impacted. After determining the length of the neck, the joint reduction shall be performed.
-
After thorough washing of the surgical area, the wound is closed, leaving a drain to evacuate a possible haematoma.
-
A sterile dressing will end the surgery and the patient will be transferred to the resuscitation area until the anaesthetist determines when the patient can return to the ward.
-
The duration of the surgical procedure is approximately one hour. The patient will be in the operating theatre from the time he/she enters the pre-anaesthesia area to the time he/she leaves the resuscitation area, between 3 and 4 hours. Before being taken to their room, they will undergo a radiological check-up by the Radiology Department.
Ergebnis einer Hüftgelenkersatzoperation:
Vorher und Nachher
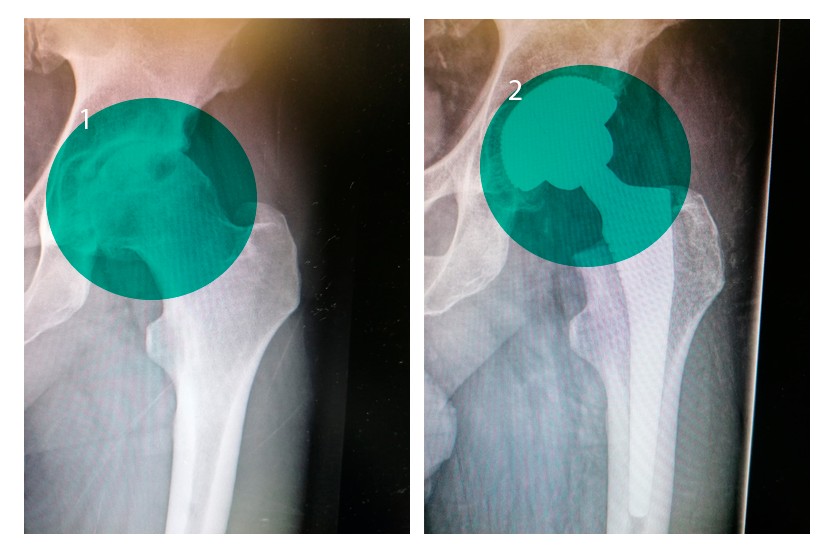
Recovery Phase
From the radiology department, the patient is transferred to his or her room on the hospital ward, where he or she will stay for 3 to 4 days.
On the first day after surgery, a new control blood test will be performed. In the rare case of a drop in haemoglobin, the blood we have in reserve for each patient will be used.
Also on this first day, the bladder catheter and drainage will be removed, and thefirst treatment will be performed.
From this first day after surgery, the patient will be mobilised with a walker or crutches, this EARLY MOBILISATION being very important to avoid complications. The patient will be able to progressively load and move the joint below the pain.
The Physiotherapy Service will be responsible for teaching the patient to walk with crutches or a walker, so that, on the third or fourth day, the patient will be able to walk independently and can be discharged from hospital.
It is important to start movement and rehabilitation exercises as soon as possible, as this will significantly shorten recovery times, as well as the possibility of complications.
At home, the patient must continue with daily dressings of the surgical wound, so that after approximately twelve days the staples that close the wound can be removed.
How soon will I be able to return to work after surgery?
The time to return to work will depend directly on the type of work performed.
-
In the case of sedentary office work, the patient will be able to return to work about 2 months after surgery.
-
Whereas, if it is a work that requires a high physical effort, the waiting time can be extended to between 4 and 6 months.
Clinic stay: <3-4 days.
Duration of surgery: 1 hour.
Anaesthesia: Raquidea.
Hip prosthesis included: Yes
Full recovery: 3 months.
Price of a hip prosthesis operation in Palma de Mallorca
The price of the hip prosthesis operation by the Prosthetic Surgery Unit with Dr. Fernando Muñoz, is closed.
Everything is included in the price of the hip replacement operation:
-
Booking and use of the operating theatre.
-
Single room with accompanying bed. Food and hospitality for the patient.
-
Complete pre-operative.
-
Post-operative visits until medical discharge.
-
Medical fees.
-
Anaesthesiologist fees.
-
Fees for nursing staff.
-
Surgical material necessary for the operation.
-
Hip prostheses from ZIMMER & DePuy Synthes, world leaders in orthopaedics and traumatology.
-
Anaesthesia, haemotherapy-transfusions, recovery room booking, etc.
-
Medical complications insurance.


